The Kharrazian Institute Program:
The Four-Pillar Clinical Training System
The Kharrazian Institute's educational platform is built on four integrated pillars designed to develop practitioners' unparalleled, real-life clinical skills in functional medicine.
Foundational Courses

The 19 Foundational Courses taught by Dr. Datis Kharrazian provide the essential knowledge base and system integration skills needed to understand complex chronic conditions.
Monthly Expert Speaker Classes

Monthly Master Classes feature real-world clinical strategies from leading functional medicine experts, keeping your knowledge current and cutting-edge.
Clinical Grand Rounds Program

Over 100 hours of live-case grand rounds, practice management interviews, and physical exams and lab analysis.
Peer-to-Peer Community Support

A collaborative professional network offering peer case discussion, live mentorship, clinical guidance, and long-term practitioner support.
Choose How You Want to Begin
Explore the platform risk-free or unlock full access to our complete functional medicine learning experience.

Foundational Courses
(19 courses = 200 hours) by Dr. Datis Kharrazian
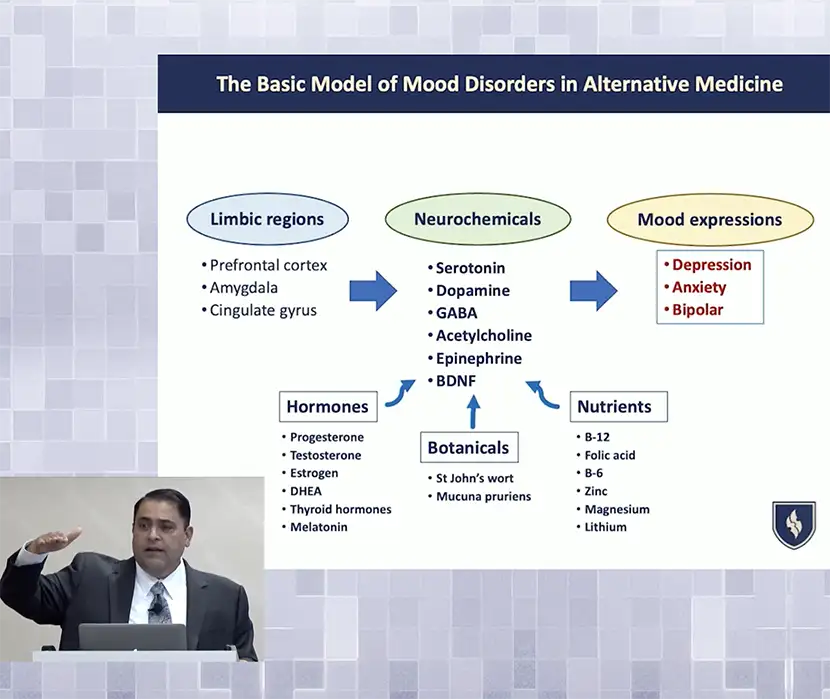
The Kharrazian Institute foundational courses, led by world-renowned functional medicine practitioner, Dr. Datis Kharrazian, offer the definitive pathway to mastering complex chronic cases.
This comprehensive collection of 19 courses—spanning critical topics like autoimmunity, cognitive disorders, chronic infections, gastrointestinal health, and hormone imbalances—moves beyond isolated protocols to teach the single most essential skill in functional medicine: system integration. Each course is a deep dive into evidence-based clinical models, enriched with real-life case studies, lab interpretation pearls, and proven treatment strategies.
You don't just learn about a condition; you learn how to identify and address its roots across multiple physiological systems, transforming your ability to treat the "mystery" cases that conventional medicine often leaves unsolved.
Whether you choose to focus on a specific challenge with an individual course or commit to the complete curriculum, you are investing in a proven clinical framework that delivers superior patient outcomes. By mastering these 19 foundational subjects, you gain a panoramic view of the body's interconnectedness, allowing you to develop truly personalized, effective treatment plans. Join the thousands of practitioners who have adopted Dr. Kharrazian's clinical models to build practices defined by clinical excellence, confidence, and mastery in managing the toughest chronic health conditions.
19 courses
Comprehensive curriculum across key clinical topics
200 hours
In-depth learning with practical clinical application
Led by Dr. Datis Kharrazian
World- renowned functional medicine practitioner
Evidence Based
Real life cases, lab pearls, and proven treatment strategies

Neuroinflammation
12 hours

Gastrointestinal Disorders
12 hours

Autoimmunity
12 hours

Hashimoto’s Hypothyroidism
12 hours

Diabetes and Dysglycemia
12 hours

Infertility, Prenatal and Maternal Health
12 hours

Cognitive Decline and Dementia
12 hours

Chronic Fatigue and Pain Syndromes
12 hours

Childhood Development
12 hours

Cardiovascular and Neurovascular Syndromes
12 hours

Mood and Anxiety
12 hours

Longevity
12 hours

Chronic Infections
12 hours

Hormone Imbalances
12 hours

Essentials of Functional Medicine
8 hours

Chronic Inflammation
6 hours

Respiratory and Sinus
6 hours

Headaches
6 hours

Degenerative Joint, Muscle and Bone Conditions
6 hours

Monthly Expert Speaker Classes
by the World’s Leading Experts in Functional Medicine

Beyond the foundational curriculum, your enrollment grants you access to our exclusive series of Monthly 5-Hour Master Classes, taught by a rotating roster of the world's leading functional medicine clinicians. These in-depth, clinically focused sessions are designed to ensure your practice remains on the cutting edge. Each expert is encouraged to share the practical, real-world protocols they use daily in their own successful practices, offering diverse perspectives and filling any knowledge gaps not covered in the core program. This commitment to constantly evolving content and bringing in new clinical voices means that as a Kharrazian Institute member, you are positioned at the forefront of the field.
You don't just learn established models; you become an active participant in the constant evolution of functional medicine, ensuring your skills and strategies are always the most current and comprehensive available.
Monthly Masterclasses
5-hour in-depth sessions
World Class Experts
Rotating roaster of leading clinicians
Real World Protocols
Practical strategies you can apply immediately
Always Current
New topics, new voices, and constant evolution

Clinical Grand Rounds Program
Achieve Clinical Mastery
For the ultimate development of your functional medicine expertise, the Kharrazian Institute offers the exclusive Clinical Mastership Training Program (CMP), a robust educational track consisting of 20 separate modules and over 100 hours of specialized education.
The CMP goes far beyond foundational concepts and monthly topics to deliver a complete, practical skill-building system for the advanced clinician.
Each module of the CMP is a powerful six-part module designed to integrate every aspect of high-level practice.
20 Modules
Comprehensive structured training
100+ hours
Specialized clinical education
Real-Life Cases
Learn from complex, real-world cases
Advanced Skills
Elevate your clinical expertise with focused training
Part 1
Grand Rounds with Real-Life Clinical Cases
Step into Dr. Kharrazian's practice as he shares his entire clinical work-up and thought process for managing complex patient referrals from around the world. Observe every detail: medical history, video-based physical exams, lab analysis, multi-variable strategy development, personalized protocol design, and the full arc of the patient journey—including follow-up modifications and a transparent view of real-life clinical outcomes.
Part 2
Clinical Expert Interviews
Dr. Kharrazian opens his personal network, bringing you direct, in-depth interviews with leading researchers and distinguished clinicians to share their specific expertise.
Part 3
Practice & Lifestyle Management Interviews
Learn the essential, non-clinical skills necessary for long-term success. Successful practitioners share their lessons on avoiding burnout, managing a thriving clinic, and achieving balance amidst the demands of a busy functional medicine practice.
Part 4-6
Specialized Training Videos
Sharpen your technical skills with focused training on Physical Examination techniques to generate key clinical information, Laboratory Interpretation to build your diagnostic and ordering prowess, and dedicated modules on improving complex Clinical Management protocols.
Module 1: Autoimmune vascular disease case
Clinical Mastership Module 1
Autoimmune vascular disease case
Case Study Grand Rounds:
48-year-old female patient that had a recent heart attack. A carotid stent injury caused significant damage to her coronary artery due to underlying autoimmunity of her vascular connective tissue that was unknown at the time of the procedure. She was later diagnosed with mixed connective tissue autoimmunity and Systemic Lupus Erythematosus. She sought out care with Dr. Kharrazian to help find diet, nutrition, and lifestyle strategies to improve her health, help her cardiovascular recovery, and find ways to dampen her autoimmune response.

Clinical Expert Topic Interview: Stephanie Seneff, PhD
We discuss the herbicide glyphosate.

Practice and Lifestyle Interview: Chris Turnpaugh, DC
We discuss multi-disciplinary functional medicine clinics.
Physical Examination Skills:
Evaluation of circulation
Laboratory Interpretation Clinical Skill:
Serum 25-hydroxy vitamin D and 1,25 dihydroxy vitamin D during infection and autoimmune responses
Clinical Management Clinical Pearl:
Clinical practice visual audit
Module 2: Post-Ramsay Hunt with exhaustion and dizziness
Clinical Mastership Module 2
Post-Ramsay Hunt with exhaustion and dizziness
Case Study Grand Rounds:
involves a case of a 75-year-old female suffering from severe exhaustion and dizziness after a viral infection into the brainstem and cranial nerves (Ramsey-Hunt Syndrome) from 4 years ago.

Clinical Expert Topic Interview: Michael Stone, MD
We discuss how do you know where to start when developing a treatment strategy.

Practice and Lifestyle Interview: Tim Katke
As vice president of Apex Energetics, Tim has developed relationships with hundreds of successful clinicians over the past 40 years. In this interview, we discuss what factors he has found that make clinical practices successful and what he has noticed that leads practitioners to fail in practice or burn out.
Physical Examination Skills:
Thyroid physical exam (inspection, auscultation, and palpation)
Laboratory Interpretation Clinical Skill:
Serum Platelets and thrombocytosis as a red flag
Clinical Management Clinical Pearl:
he importance of implementing and enforcing appointment cancelation fees.
Module 3: Chronic gastrointestinal issues
Clinical Mastership Module 3
Chronic gastrointestinal issues
Case Study Grand Rounds:
33-year-old male with chronic gastrointestinal dysfunction for 10 years with limited clinical outcomes to dietary changes and nutraceutical supplements.

Clinical Expert Topic Interview: Joseph Pizzorno, ND
We discuss clinical applications for persistent and non- persistent toxic chemicals.

Practice and Lifestyle Interview: Shane Steadman, DC, DACNB, CNS
How to develop a successful chronic disease practice
Physical Examination Skills:
Upper motor neuron lesions exam
Laboratory Interpretation Clinical Pearl:
Macrocytosis
Clinical Management Clinical Pearl:
Staying on time with your patients/clients
Module 4: Anxiety and panic attacks
Clinical Mastership Module 4
Anxiety and panic attacks
Case Study Grand Rounds:
17-year-old female patient with chief complaints of anxiety and panic attacks.

Clinical Expert Topic Interview: Liz Lipski, PhD, FACN, CNS
How to manage complex gastrointestinal issues.

Practice and Lifestyle Interview: Eric Dorninger, ND, LAc
Real-life tips to help run a successful chronic disease practice and how to balance it with one’s personal and family life.
Physical Examination Skills:
Olfactory examination
Laboratory Interpretation Clinical Skill:
Understanding serum iron markers
Clinical Management Clinical Pearl:
Knowing when it is time to refer
Module 5: Gut, pain and brain issues
Clinical Mastership Module 5
Gut, pain and brain issues
Case Study Grand Rounds:
47-year-old patient with chronic gastrointestinal bloating, chronic anxiety, chronic pain, and progressive loss of memory.

Clinical Expert Topic Interview: Monique Class, MS, APRN, BC
How to effectively communicate your clinical goals with patients/clients.

Practice and Lifestyle Interview: Kristi Hughes, ND
Variables that facilitate transitioning into a good functional medicine practitioner.
Physical Examination Skills:
Evaluation of muscle tone.
Laboratory Interpretation Clinical Skill:
Acute phase reactants.
Clinical Management Clinical Pearl:
Patients who cannot comply with care.
Module 6: Chronic pain, weakness and migraines
Clinical Mastership Module 6
Chronic pain, weakness and migraines
Case Study Grand Rounds:
64-year-old female with chief complaints of chronic systemic body pain, weakness and swelling in legs, headaches, migraines, heartburn, and reoccurring episodes of dizziness.

Clinical Expert Topic Interview: Akil Palanisamy, MD
The impact of phytochemicals and spices on the microbiome and how to use stool analysis labs in clinical practice.

Practice and Lifestyle Interview: Ionela Hubbard, MD, LAc
Loma Linda University School of Medicine
Physical Examination Skills:
Finger-targeting testing
Laboratory Interpretation Clinical Skill:
Understanding B12 and folate serum markers
Clinical Management Clinical Pearl:
Patient input
Module 7: Parkinson’s Disease
Clinical Mastership Module 7
Parkinson’s Disease
Case Study Grand Rounds:
A 61-year-old female patient was diagnosed with Parkinson’s Disease and progressive dystonia and stiffness. She has also recently developed anxiety and panic attacks.

Clinical Expert Topic Interview: Anil Bajnath, MD
In this interview we discuss Dr. Bajnath’s journey into function and precision medicine. We also discuss the use of biohacking in combination with functional medicine.

Practice and Lifestyle Interview: Kat Toups, MD
In this interview, we discuss the challenges of working with patients suffering from cognitive decline.
Physical Examination Skills:
Neurological handwriting evaluation.
Laboratory Interpretation Clinical Skill:
Serum protein electrophoresis as an effective method for general surveillance of underlying pathophysiology.
Clinical Management Clinical Pearl:
Case management with an unsupportive spouse.
Bonus Videos:
How to avoid the pitfalls of burnout when working with chronic disease, how to properly communicate with patients who have incurable conditions, how not to base self-worth on patient outcomes, and how to develop a “real” rest day to recover each week.
Module 8: Pre-conception fatigue and health issues
Clinical Mastership Module 8
Pre-conception fatigue and health issues
Case Study Grand Rounds:
A 35-year-old female patient suffering from chronic fatigue, anxiety, depression, and asthma. She wants to improve her symptoms and optimize her health for pregnancy.

Clinical Expert Topic Interview: Aimie Apigian, MD, MS, MPH
In this interview we discuss Dr. Bajnath’s journey into function and precision medicine. We also discuss the use of biohacking in combination with functional medicine.

Practice and Lifestyle Interview: David Musnick, MD
In this interview, we discuss how he transitioned from conventional medicine into functional medicine. The importance of patient education, physical examination, and patient handouts. He discusses what he has learned in consulting and educating patients and provides multiple clinical pearls.
Physical Examination Skills:
Evaluation of auditory pathways and their significance in clinical practice.
Laboratory Interpretation Clinical Skill:
Anemia due to chronic inflammation also known as anemia of chronic disease.
Clinical Management Clinical Pearl:
How to determine the frequency of patient follow-ups when managing a case.
Bonus Videos:
How to understand the clinical thought process versus protocols, the importance of basic diagnosis, and the importance of understanding basic human physiology.
Module 9: Hashimoto’s and low blood pressure
Clinical Mastership Module 9
Hashimoto’s and low blood pressure
Case Study Grand Rounds:
A 51-year-old female patient suffering from Hashimoto’s, anxiety, insomnia, episodes of depression and extreme fatigue, brain fog, body zaps, neck pulsations, and very low blood pressure.

Clinical Expert Topic Interview: Jeffery Bland, PhD
In this interview, we talk about the development of functional medicine, the principles of functional medicine, and the attributes necessary to be a good functional medicine practitioner.

Practice and Lifestyle Interview: Linda Clark, MA, CNC
In this interview, we discuss the role of a clinical nutritionist in the field of functional medicine..
Physical Examination Skills:
Ophthalmoscopy and its significance in a chronic disease clinical practice.
Laboratory Interpretation Clinical Skill:
Evaluation of cortisol salivary profiles and the cortisol awakening response.
Clinical Management Clinical Pearl:
How to determine the atmosphere of your front office and staff.
Bonus Videos:
Don’t compare yourself to other clinicians, look at old patient/client files to determine if you are growing, and don’t get scattered with your clinical education.
Module 10: Post radioactive iodine therapy issues
Clinical Mastership Module 10
Post radioactive iodine therapy issues
Case Study Grand Rounds:
A 35-year-old female was diagnosed with Grave’s disease and treated with radioactive iodine therapy. Post-treatment she had ongoing symptoms of both hypothyroidism and hyperthyroidism. In recent years she has developed cognitive impairment, reduced stamina, and systemic inflammation.

Clinical Expert Topic Interview: Terry Wahls, MD
In this interview, we talk about the functional medicine approaches to multiple sclerosis and autoimmune diseases.

Practice and Lifestyle Interview: Mark Holthouse, MD
In this interview, we discuss how he transitioned from conventional medicine into a successful functional medicine practice.
Physical Examination Skills:
Ophthalmoscopy and its significance in a chronic disease clinical practice.
Laboratory Interpretation Clinical Skill:
Evaluation of cortisol salivary profiles and the cortisol awakening response.
Clinical Management Clinical Pearl:
How to determine the atmosphere of your front office and staff.
Bonus Videos:
Don’t compare yourself to other clinicians, look at old patient/client files to determine if you are growing, and don’t get scattered with your clinical education.
Module 11: Lifelong gastrointestinal issues
Clinical Mastership Module 11
Lifelong gastrointestinal issues
Case Study Grand Rounds:
Toby is a 28-year-old male suffering from chronic gastrointestinal problems. His gastrointestinal symptoms of constant bloating and pain started in high school and progressed into college and his adult life. He has been evaluated by many gastroenterologists, nutritionists, and functional medicine practitioners.

Clinical Expert Topic Interview: Mark Newman, MS
President and founder of Precision Analytical Inc. and developer of the dried urine test for comprehensive hormones (DUTCH) test.

Practice and Lifestyle Interview: Pedrom Shojai, OMD
Doctor of Chinese medicine and author of the New York Times best-selling author of the Urban Monk, Rise and Shine, and the Art of Stopping Time.
Physical Examination Skills:
How to identify brain-based physical injuries during the physical examination.
Laboratory Interpretation Clinical Skill:
Evaluation and applications of serum lipid phenotype testing.
Clinical Management Clinical Pearl:
How to develop a clinical management plan with your patient’s budget.
Bonus Videos:
Making time to study, starting a case all over, refining your physical exam skills
Module 12: Bipolar disorder
Clinical Mastership Module 12
Bipolar disorder
Case Study Grand Rounds:
Ali is a 42-year-old male suffering from bipolar disorder, chronic gastrointestinal difficulties, fatigue, depression, and brain fog. Over the years, he has made many adjustments to his diet and has tried numerous nutraceuticals to help his symptoms with limited clinical impacts.

Clinical Expert Topic Interview: Chad Larson, NMD, DC, CCN, CSCS
In this interview, we discuss dietary factors that promote chronic pain. Interview topics include the ketogenic diet, vegan diets, vegetarian diets, protein requirements for recovery, blood sugar stability, inflammatory triggers, hydration, and various applications to unwind patients with chronic pain.

Practice and Lifestyle Interview: Elizabeth Bradley, MD
In this interview, we discuss the Center for Functional Medicine at the Cleveland Clinic and how those practicing functional medicine in conventional medical centers can implement functional medicine principles into their clinical environment.
Physical Examination Skills:
How to evaluate brain-gut axis dysfunction with a physical examination.
Laboratory Interpretation Clinical Skill:
Evaluation of saliva IgA multiple mucosal immune reactivity panel (Cyrex Array 14)
Clinical Management Clinical Pearl:
How to work through a clinical case.
Bonus Videos:
How to handle patients with nutraceutical sensitivities, don’t talk politics to your patients, and don’t share your personal problems with your patients.
Module 13: Tinnitus and multiple symptoms
Clinical Mastership Module 13
Tinnitus and multiple symptoms
Case Study Grand Rounds:
Zeba is a 69-year-old female with diverse sensations of hot and cold throughout her body. She has tinnitus, chronic gastrointestinal symptoms, and a medical history of many diverse and unclear symptoms.

Clinical Expert Topic Interview: Mimi Guarneri, MD, FACC, ABOIM
Board-certified in Cardiovascular Disease, Internal Medicine, and Integrative Holistic Medicine. We discuss her opinions on various diets, nutraceuticals, and lifestyle applications for vascular health. We also discuss how to evaluate cardiovascular disease with physical examination, blood tests.

Practice and Lifestyle Interview: Blake Ambridge DC, DACNB
He has spent 35 years in private practice. In this interview, we discuss clinical issues such as reducing patient fees, sponsoring patients, how to stay on time, practice overhead, and how to stay efficient in clinical practice. Dr. Ambridge discusses important lessons that he has learned that have helped him have a successful practice.
Physical Examination Skills:
How to perform and interpret physical examination of the abdomen.
Laboratory Interpretation Clinical Skill:
The influence of hypothyroidism on other laboratory biomarkers.
Clinical Management Clinical Pearl:
The concept of trial and error in clinical practice.
Bonus Videos:
Letting the public know what you do to build your practice with books, podcasts, and social media.
Module 14: Chronic fatigue
Clinical Mastership Module 14
Chronic fatigue
Case Study Grand Rounds:
Colin is a 27-year-old male patient suffering from chronic fatigue, maldigestion, depression, and anxiety. He has symptoms of fatigue 90% of the time and feels much worse after exercise.

Clinical Expert Topic Interview: Andrew Campbell, MD
In this interview, we discuss the role of toxic mold in autoimmune and chronic diseases, how to evaluate mold toxicity in clinical practice, and treatment applications for mold illness.

Practice and Lifestyle Interview: Josh Redd, DC, MS, MPH
In this interview, we discuss how Dr. Redd has built seven successful functional medicine practices in the western US. He shares the lessons he has learned over the past 16 years working with his associates, staff, and patients.
Physical Examination Skills:
How to evaluate and interpret imbalances in visual tracking of the eyes.
Laboratory Interpretation Clinical Skill:
Identifying ominous patterns on routine blood tests.
Clinical Management Clinical Pearl:
When to call it quits when a patient does not respond to treatment strategies.
Bonus Videos:
Change your schedule to accommodate changes in your life.
Module 15: Cognitive fatigue and physical weakness
Clinical Mastership Module 15
Cognitive fatigue and physical weakness
Case Study Grand Rounds:
Mary is a 39-year-old female patient complaining of physical fatigue, general weakness, hypothyroidism, chronic parasitic infections, and severe cognitive fatigue.

Clinical Expert Topic Interview: Bryan Stepanenko, MD, MPH
In this interview, we discuss his work with implementing functional medicine strategies with soldiers that have suffered from traumatic brain injuries in the military medical system.

Practice and Lifestyle Interview: Steve Noseworthy, DC, DACNB
In this interview, we discuss his transition from a brick-and-mortar practice to a virtual practice. He will share with us how his practice works and how somebody can transition into virtual practice.
Physical Examination Skills:
How to evaluate numbness in the hands associated with thoracic outlet syndrome.
Laboratory Interpretation Clinical Skill:
Clinical application of the homeostatic model for insulin resistance (HOMA-IR).
Clinical Management Clinical Pearl:
Restricting specific conditions into your clinical practice.
Bonus Videos:
Identifying your own clinical bias.
Module 16: EMF sensitivity and multiple symptoms
Clinical Mastership Module 16
EMF sensitivity and multiple symptoms
Case Study Grand Rounds:
Vera is a 62-year-old female patient suffering from acute bouts of trembling sensation, changes in voice strength, burping attacks, weakness, and mental fatigue. She has hypersensitivities to EMFs and struggles with chronic insomnia and gastrointestinal symptoms.

Clinical Expert Topic Interview: Dr. Carrie Jones, ND, MPH
In this interview we discuss hormone and hormone profiles. Topics include the adrenal salivary index, cortisol awakening response, DUTCH testing, serum testing, saliva hormones, and more. We also discuss lab ranges and how various types of hormone replacement may impact laboratory profiles..

Practice and Lifestyle Interview: Dr. Mark Flannery, DC, CNS
In this interview, we discuss how he built a waiting list functional medicine practice.
Physical Examination Skills:
How to evaluate the skin and its implications in a functional medicine evaluation.
Laboratory Interpretation Clinical Skill:
How to evaluate a complete thyroid panel step-by-step.
Clinical Management Clinical Pearl:
Discussing prognosis and the balance between optimism and pessimism.
Bonus Videos:
Online practice resources to support your practice such as Rupa and Fullscript.
Module 17: Benzodiazepine withdrawal syndrome
Clinical Mastership Module 17
Benzodiazepine withdrawal syndrome
Case Study Grand Rounds:
Deborah is a 75-year-old female patient suffering from severe episodes of abdominal pain, insomnia, fatigue, vertigo, and benzodiazepine withdrawal syndrome. She suffers from daily episodes of anxiety, dizziness, and abnormal limb muscle movements.

Clinical Expert Topic Interview: Dr. Deanna Minich, PhD, FACN, CNS
In this interview, we discuss the role of phytonutrients as antioxidants, signaling agents, and microbiome modulators and their impact on health and disease. We discuss how lab tests can and cannot measure oxidative stress, the controversies of phytonutrients, and how phytonutrients can be used in clinical settings

Practice and Lifestyle Interview: Dr. Shlipa Sexena, MD
In this interview, we discuss group visits and her work as a chief medical officer at Forum Health, a national multi-center integrative medicine network. We also discuss how she transitioned into a successful functional medicine practice..
Physical Examination Skills:
How to identify Parkinson’s Early.
Laboratory Interpretation Clinical Skill:
How to evaluate serum renal markers and urinalysis
Clinical Management Clinical Pearl:
Addressing issues with patient complaints.
Bonus Videos:
Asking your patients to teach you.
Module 18: Chronic dysbiosis and fatigue
Clinical Mastership Module 18
Chronic dysbiosis and fatigue
Case Study Grand Rounds:
Alica is a 50-year old female patient suffering from chronic dysbiosis and fatigue.

Clinical Expert Topic Interview: Heather Sandison, ND
In this interview we discuss how she has organized a senior living facility for patients that suffer with cognitive decline, and how she is implementing functional medicine approaches in her facility to help them.

Practice and Lifestyle Interview: Yousef Elyaman, MD
In this interview we discuss how he has built a large integrative and functional medicine center with multiple practitioners and staff
Physical Examination Skills:
How to perform a mouth exam.
Laboratory Interpretation Clinical Skill:
How to evaluate serum transaminases.
Clinical Management Clinical Pearl:
Addressing patient concerns for a cure.
Bonus Videos:
Using medical dictation software.
Module 19: Chilhood development disorder
Clinical Mastership Module 19
Chilhood development disorder
Case Study Grand Rounds:
Amelia is a 13-year-old girl that has been diagnosed with multiple autoimmune diseases and childhood development disorders. She exhibits impaired neurological development of her motor and sensory systems. She suffers from chronic inflammation, inattentiveness, coordination difficulties, and chronic bloating and constipation.

Clinical Expert Topic Interview: Arti Chandra, MD, MPH
In this interview we discuss the importance of healthy soil in human health and clinical strategies she uses in her practice when working with chronic patients.

Practice and Lifestyle Interview: Lucas Gafken, DC
In this interview we discuss the journey from being a new graduate to developing a successful functional medicine practice over the past 14 years.
Physical Examination Skills:
How to identify dysautonomia during a physical exam.
Laboratory Interpretation Clinical Skill:
Serum fibrinogen and prothrombin time.
Clinical Management Clinical Pearl:
Review patient files before your clinic opens.
Bonus Videos:
Be aware of your own bias with nutraceuticals.
Module 20: Multiple irresolvable symptoms
Clinical Mastership Module 20
Multiple irresolvable symptoms
Case Study Grand Rounds:
Amanda is a 39-year-old female patient with vestibular migraines, rosacea, seborrheic dermatitis, and post-surgical trigeminal neuropathy. She has had extensive medical evaluations by specialists but they have not provided her with any strategies to resolve her conditions.

Clinical Expert Topic Interview: Tom Malterre, MS, CN
In this interview we discuss the elimination diet in depth and what factors can impact success and failure with elimination diets. We also jump into the topic of migraines and functional medicine applications.

Practice and Lifestyle Interview: Thomas Culleton, DC
In this interview we discuss Dr. Culleton’s introduction and growth into functional medicine and how it impacted his private practice.
Physical Examination Skills:
How to evaluate speech and identify underlying mechanisms of dysarthria.
Laboratory Interpretation Clinical Skill:
How to evaluate the Fibrosis–4 score (FIB-4) to evaluate fibrosis with routine laboratory markers.
Clinical Management Clinical Pearl:
How to review laboratory results with your patients.
Bonus Videos:
Remember your role in patient care.

Peer-to-Peer Community Support
Join a Global Community Committed to Excellence

The final pillar of clinical training at the Kharrazian Institute is our robust Peer-to-Peer Support System. We believe that the transition from classroom theory to clinical mastery is best achieved through a global, multidisciplinary network of healthcare providers in our community. This ecosystem is powered by two distinct interactive features:
The Clinician’s Roundtable Discussion Forum: This private, members-only forum serves as your 24/7 space for peer-to-peer collaboration. Whether you are navigating your first complex case or you are a seasoned practitioner fine-tuning a sophisticated clinical strategy, the Roundtable provides the collective wisdom of our community of functional medicine clinicians to help you solve questions you may have about lab results, clinical strategies, or tips on how to improve your practice.
The Clinical Mentorship Circle Online Meeting: We facilitate live video conference meetings where peer-to-peer interaction meets expert guidance. In these sessions, we bring in expert clinicians to provide direct mentorship on everything from intricate case analysis to the practicalities of running a successful, high-impact practice. This is your opportunity to ask specific questions and have mentors to help your development.
By joining the Kharrazian Institute, you are never practicing in isolation. You are part of a dedicated community committed to supporting one another, ensuring you have a professional safety net and a trusted referral pipeline long after the lectures are over.
Clinician Roundtable
24/7 peer-to-peer case collaboration
Live Mentorship Sessions
Interactive meetings with expert clinicians
Complex Case Support
Guidance on labs, strategies, and patient care
Professional Network
Trusted referrals and lasting connections
Choose How You Want to Begin
Explore the platform risk-free
No credit card required
Or unlock full access to our complete functional medicine learning experience
$399 /per month
or
$3999 /per year
Plus a $995 one-time setup fee on the monthly plan. Save $1784 with the annual plan
Cancel anytime. Instant access.
